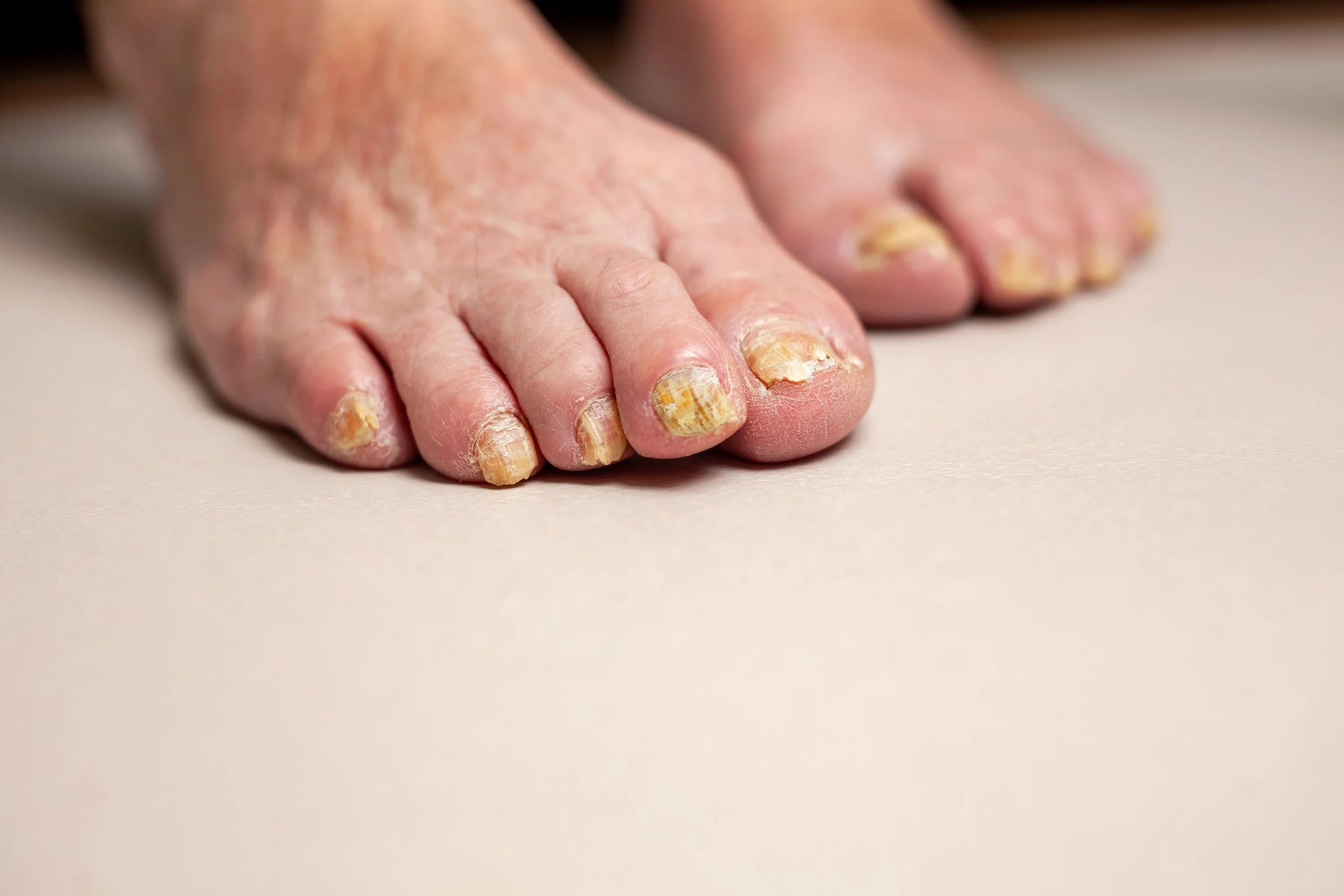
Fungal Nail Infection: What You Need to Know
Fungal nail infections are one of the most common concerns I see in clinic. They can be frustrating, slow to respond to treatment, and sometimes misunderstood.
If you’ve noticed your toenail becoming thickened, discoloured, crumbly, or lifting away from the nail bed, a fungal infection may be the cause — but it’s not always that simple.
Let’s break it down.
What Is a Fungal Nail Infection?
A fungal nail infection (onychomycosis) occurs when fungi — usually dermatophytes — invade the nail plate or nail bed. Toenails are affected far more often than fingernails due to:
Warm, enclosed footwear
Reduced circulation to the toes
Minor repetitive trauma
Slower nail growth
It’s a common condition, particularly in adults over 40.
What Does It Look Like?
Common signs include:
Yellow, white, or brown discolouration
Thickened nail plate
Crumbling or brittle edges
Nail lifting (onycholysis)
Debris under the nail
Not every thick or discoloured nail is fungal. Trauma, psoriasis, ageing, or previous nail surgery can produce similar changes. That’s why proper assessment matters.
Is It Just Cosmetic?
Many people assume fungal nails are purely aesthetic. In some cases, they may cause no pain — but they can:
Become uncomfortable in footwear
Spread to other nails
Contribute to athlete’s foot
Increase infection risk in high-risk patients (especially those with diabetes)
For some individuals, it can also significantly affect confidence.
How Is It Diagnosed?
Diagnosis is usually clinical, but in uncertain cases, nail sampling may be recommended before beginning treatment — particularly if oral medication is being considered.
Treating a nail that isn’t actually fungal wastes time and money, so clarity is important.
Treatment Options
Treatment depends on severity, symptoms, and overall health.
Topical Treatments
These are applied directly to the nail. They are most effective when:
The infection is mild to moderate
The nail matrix (growth area) is not extensively involved
They require consistency and patience — improvement takes months because nails grow slowly.
Oral Antifungal Medication
In more established infections, oral treatment may be considered. These medications work systemically and tend to have higher success rates, but require GP involvement and consideration of medical history.
Debridement (Professional Nail Reduction)
Regular reduction of thickened fungal nails by a podiatrist can:
Reduce pressure and discomfort
Improve penetration of topical treatments
Improve overall appearance
This is often a key part of management.
How Long Does It Take to Clear?
Toenails grow slowly — approximately 1–2 mm per month.
Even when treatment is effective, it can take:
9–12 months for a full toenail to grow out
Longer in some individuals
Consistency and realistic expectations are essential.
Can It Come Back?
Yes — recurrence is common.
Preventative measures include:
Keeping feet dry
Changing socks daily
Avoiding walking barefoot in communal areas
Treating athlete’s foot promptly
Disinfecting footwear where appropriate
Long-term prevention is often as important as initial treatment.
When Should You Seek Advice?
You should consider professional assessment if:
The nail is painful
The nail is thick and difficult to manage
You have diabetes or circulatory issues
Multiple nails are affected
You are unsure whether it is fungal
Early guidance can prevent the condition worsening and help you choose the most appropriate treatment pathway.
Final Thoughts
Fungal nail infections are common and manageable, but they require patience and a tailored approach. Not every thickened nail is fungal, and not every fungal nail requires aggressive treatment.
If you’re unsure, it’s always worth having it assessed. Clear advice at the outset can save months of frustration.
📍 The Glen, Main Street, Brampton, CA8 1SB
📞 016977 2191
💻 www.baileypodiatry.co.uk/book
We’re here to help you put your best foot forward — comfortably and confidently.
Bailey Podiatry & Reflexology
Supporting your foot health – and your whole wellbeing
#fungalnails #onychomycosis #foothealth #podiatryuk #nailhealth #toenailfungus #healthyfeet #preventativefootcare #diabeticfootcare #ruralhealthcare #bramptoncumbria #cumbrialife #baileypodiatryandreflexology
References
Ameen, M., Lear, J.T., Madan, V., Mohd Mustapa, M.F. and Richardson, M. (2014) ‘British Association of Dermatologists’ guidelines for the management of onychomycosis 2014’, British Journal of Dermatology, 171(5), pp. 937–958.
Gupta, A.K., Mays, R.R., Versteeg, S.G., Piraccini, B.M., Shear, N.H. and Piguet, V. (2018) ‘Update on current approaches to diagnosis and treatment of onychomycosis’, Expert Review of Anti-infective Therapy, 16(12), pp. 929–938.
Lipner, S.R. and Scher, R.K. (2019) ‘Onychomycosis: Clinical overview and diagnosis’, Journal of the American Academy of Dermatology, 80(4), pp. 835–851.
NICE (2022) Fungal nail infection. National Institute for Health and Care Excellence. Available at: https://cks.nice.org.uk (Accessed: 13 February 2026).
Thomas, J., Jacobson, G.A., Narkowicz, C.K., Peterson, G.M., Burnet, H. and Sharpe, C. (2010) ‘Toenail onychomycosis: An important global disease burden’, Journal of Clinical Pharmacy and Therapeutics, 35(5), pp. 497–519.